Introduction
Our department has collaborated with different clinical and non-clinical departments on children’s research involving imaging. The following are some examples of key areas of research.
Imaging of new pediatric disorders
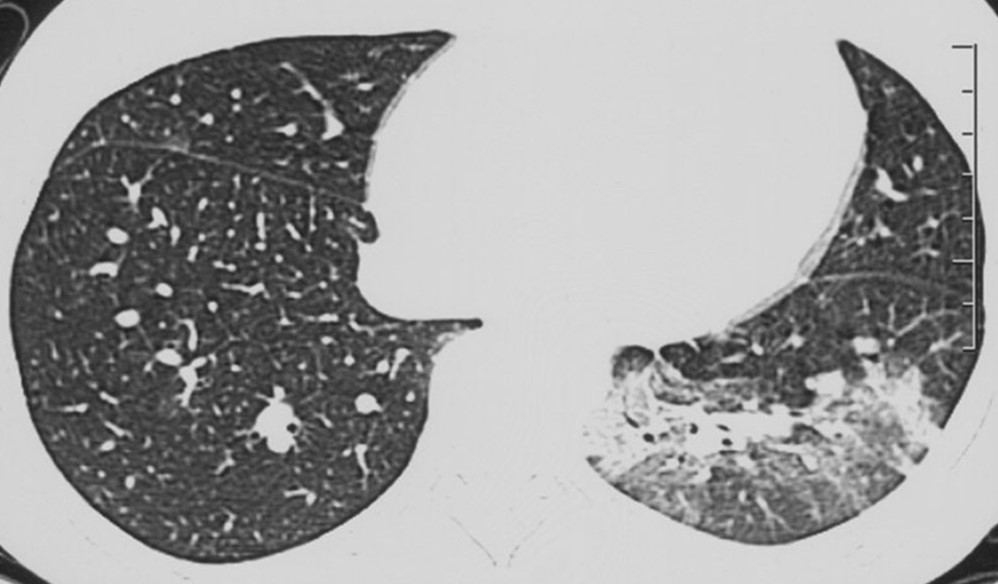
- CUHK Radiology is first group describing the initial chest radiographic and high-resolution CT thorax findings of severe acute respiratory syndrome (SARS). Recently, we also collaborated with other researchers worldwide and published articles related to COVID-19.
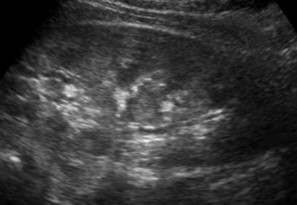
- We are also the first group to report ultrasonographic findings of kidney in children exposed to melamine-tainted milk products. During the past decade, our research team has been at the forefront of investigating imaging characteristics of new paediatric disorders, contributing to timely and accurate diagnosis as well as optimizing patient management.
Representative publications:
- Foust AM, Winant AJ, Chu WC, Das KM, Phillips GS, Lee EY. Pediatric SARS, H1N1, MERS, EVALI, and Now Coronavirus Disease (COVID-19) Pneumonia: What Radiologists Need to Know. AJR Am J Roentgenol. 2020;215(3):736-744.
- Ho SS, Chu WC, Wong KT, Li CK, Wong W, Ng PC, Ahuja AT. Letter to editor: Ultrasonographic evaluation of melamine-exposed children in Hong Kong. N Engl J Med. 2009;360(11):1156-7.
- Chu WC, Li AM, Ng AW, So HK, Lam WW, Lo KL, Yeung MC, Yau YS, Chiu WK, Leung CW, Ng PC, Hon KL, Mo KW, Fok TF, Ahuja AT. Thin-Section CT 12 Months After the Diagnosis of Severe Acute Respiratory Syndrome in Pediatric Patients. AJR Am J Roentgenol. 2006;186(6):1707-14.
- Hon KL, Leung CW, Cheng WT, Chan PK, Chu WC, Kwan YW, Li AM, Fong NC, Ng PC, Chiu MC, Li CK, Tam JS, Fok TF. Clinical presentations and outcome of severe acute respiratory syndrome in children. Lancet. 2003;361(9370):1701-3.
Imaging in Adolescent Idiopathic Scoliosis (AIS)
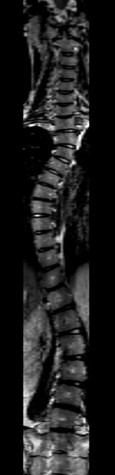
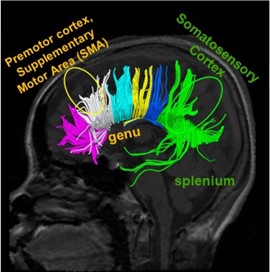
Our research team is the group which has published the largest number of MRI-related research on AIS. Comprehensive imaging studies have been carried out to investigate the etiopathogenesis of Adolescent Idiopathic Scoliosis (AIS). Studies involved the use of different imaging modalities included diffusion tensor imaging in MRI, CT and bi-planar radiography to study the fiber tracks, morphology and mechanical properties of the spine, intervertebral discs, brain and lung morphology in patients with AIS. Recently we collaborated with other international groups to predict the curve progression in AIS patients based on scoliotic curve morphology reconstructed from low-dose biplanar radiography and 3D ultrasound.
Representative publications:
- Pang H, Wong YS, Yip BH, Hung AL, Chu WC, Lai KK, Zheng YP, Chung TW, Sharma G, Cheng JC, Lam TP. Using Ultrasound to Screen for Scoliosis to Reduce Unnecessary Radiographic Radiation: A Prospective Diagnostic Accuracy Study on 442 Schoolchildren. Ultrasound Med Biol. 2021;47(9):2598-2607.
- Vergari C, Skalli W, Abelin-Genevois K, Bernard JC, Hu Z, Cheng JCY, Chu WCW, Assi A, Karam M, Ghanem I, Bassani T, Galbusera F, Sconfienza LM, Brayda-Bruno M, Courtois I, Ebermeyer E, Vialle R, Langlais T, Dubousset J. Effect of curve location on the severity index for adolescent idiopathic scoliosis: a longitudinal cohort study. Eur Radiol. 2021;31(11):8488-8497.
- Xue C, Shi L, Hui SCN, Wang D, Lam TP, Ip CB, Ng BKW, Cheng JCY, Chu WCW. Altered White Matter Microstructure in the Corpus Callosum and Its Cerebral Interhemispheric Tracts in Adolescent Idiopathic Scoliosis: Diffusion Tensor Imaging Analysis. AJNR Am J Neuroradiol. 2018;39(6):1177-1184.
- Hui SC, Pialasse JP, Wong JY, Lam TP, Ng BK, Cheng JC, Chu WC. Radiation dose of digital radiography (DR) versus micro-dose x-ray (EOS) on patients with adolescent idiopathic scoliosis: Scoliosis Spinal Disord. 2016;11:46.
SOSORT- IRSSD “John Sevastic Award” Winner in Imaging Research. - Kong Y, Shi L, Hui SC, Wang D, Deng M, Chu WC, Cheng JC. Variation in anisotropy and diffusivity along the medulla oblongata and the whole spinal cord in adolescent idiopathic scoliosis: a pilot study using diffusion tensor imaging. AJNR Am J Neuroradiol. 2014;35(8):1621-7.
- Chu WC, Rasalkar DD, Cheng JC. Asynchronous neuro-osseous growth in adolescent idiopathic scoliosis–MRI-based research. Pediatr Radiol. 2011;41(9):1100-11.
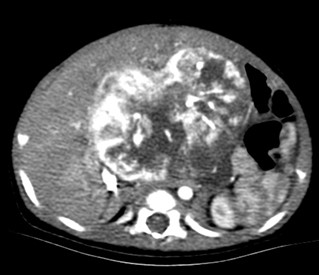
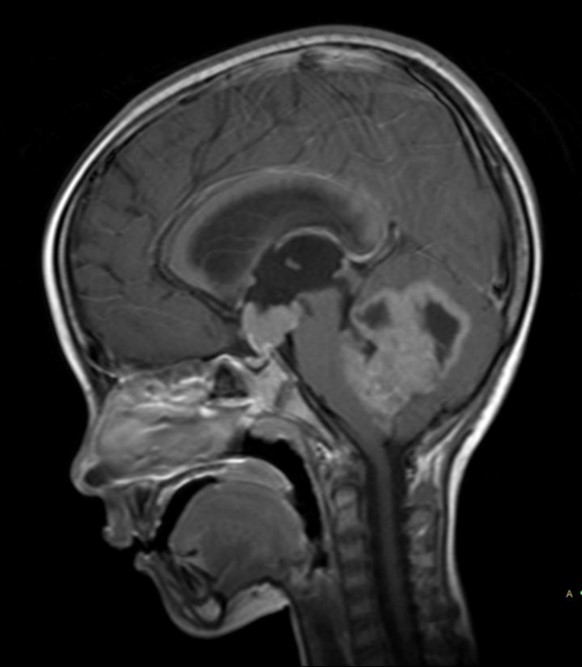
Imaging of paediatric oncology patients and organ iron load in thalassemia patients
Our group has published imaging findings in various paediatric CNS, thoracic and abdominal malignancy. We collaborated with National Heart and Lung Institute, Imperial College London, UK to validate T2* protocol for quantitative assessment of hepatic and cardiac load in various organs in thalassaemia major patients who receive regular blood transfusion. This technique now becomes the standard of care for clinical management in thalassaemia patients.
Representative publications:
- Rasalkar DD, Chu WC, Lee V, Paunipagar BK, Cheng FW, Li CK. Pulmonary metastases in children with osteosarcoma: characteristics and impact on patient survival. Pediatr Radiol. 2011;41(2):227-36.
- Rasalkar DD, Chu WC, Cheng FW, Paunipagar BK, Shing MK, Li CK. Atypical location of germinoma in basal ganglia in adolescents: radiological features and treatment outcomes. Br J Radiol. 2010;83(987):261-7.
- Leung AW, Chu WC, Lam WW, Lee V, Li CK. Magnetic resonance imaging assessment of cardiac and liver iron load in transfusion dependent patients. Pediatr Blood Cancer. 2009;53(6):1054-9.
- He T, Kirk P, Firmin DN, Lam WM, Chu WC, Au WY, Chan GC, Tan RS, Ng I, Biceroglu S, Aydinok Y, Fogel MA, Cohen AR, Pennell DJ. Multi-center transferability of a breath-hold T2 technique for myocardial iron assessment. J Cardiovasc Magn Reson. 2008;10(1):11.
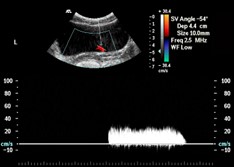
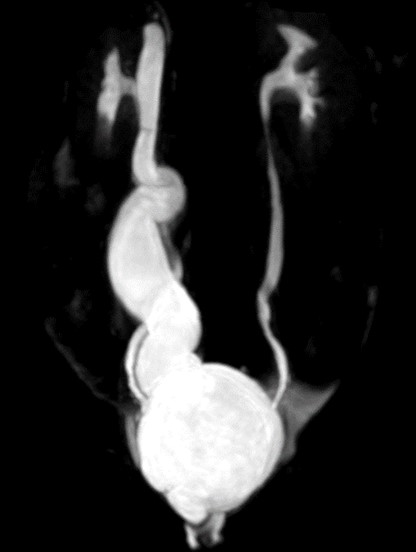
Dynamic and Doppler Ultrasound Studies of Urinary Tracts in Children and Foetuses
Our research team is the first group to develop dynamic imaging protocol for urinary bladder and assess ureteric waves using Colour Doppler imaging with an invited review article published on the above topic. The technique is now being used to guide clinical management in our institution.
Representative publications:
- Leung VY, Chu WC, Metreweli C. Hydronephrosis index: a better physiological reference in antenatal ultrasound for assessment of fetal hydronephrosis. J Pediatr. 2009;154(1):116-20.
- Leung VY, Chu WC, Yeung CK, Metreweli C. Doppler waveforms of the ureteric jet: an overview and implications for the presence of a functional sphincter at the vesicoureteric junction. Pediatr Radiol. 2007;37(5):417-25.
Chosen for CME accreditation - Leung VY, Chu WC, Yeung CK, Metreweli C. Ureteric jet Doppler waveform and bladder wall thickness in children with nocturnal enuresis. Pediatr Res. 2006;60(5):582-6.
Selected as Editorial Focus
Application of Advanced Imaging Technique in Childhood Obesity and Liver Imaging
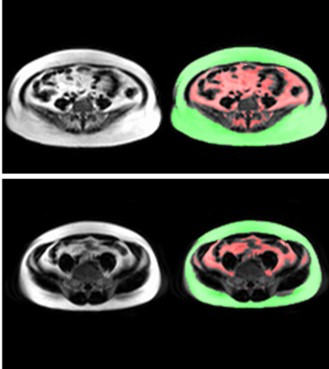
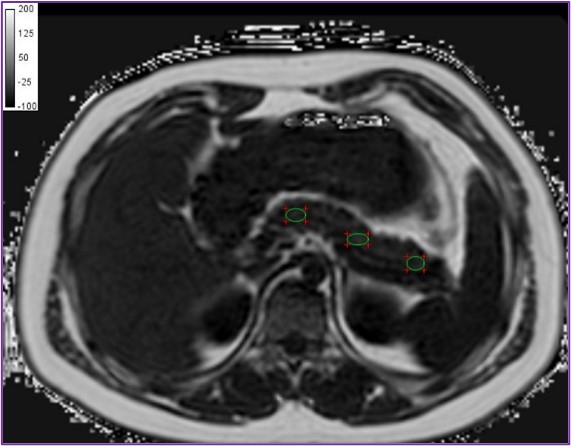
Our research team applies advanced MR water-fat & T2* imaging and MR spectroscopy for assessment of central obesity, ectopic body fat and related condition such as non-alcoholic fatty liver disease (NAFLD) and pancreatic steatosis.
Representative publications:
- Chiyanika C, Chan DFY, Hui SCN, So HK, Deng M, Yeung DKW, Nelson EAS, Chu WCW. The relationship between pancreas steatosis and the risk of metabolic syndrome and insulin resistance in Chinese adolescents with concurrent obesity and non-alcoholic fatty liver disease. Pediatr Obes. 2020;15(9):e12653.
- Hui SCN, Wong SKH, Ai Q, Yeung DKW, Ng EKW, Chu WCW. Observed changes in brown, white, hepatic and pancreatic fat after bariatric surgery: Evaluation with MRI. Eur Radiol. 2019;29(2):849-856.
- Hui SCN, So HK, Chan DFY, Wong SKH, Yeung DKW, Ng EKW, Chu WCW. Validation of water-fat MRI and proton MRS in assessment of hepatic fat and the heterogeneous distribution of hepatic fat and iron in subjects with non-alcoholic fatty liver disease. Eur J Radiol. 2018;107:7-13.
- Chan DFY, So HK, Hui SCN, Chan RSM, Li AM, Sea MM, Chu WCW, Chan M, Woo J, Nelson EAS. Dietitian-led lifestyle modification programme for obese Chinese adolescents with non-alcoholic fatty liver disease: a randomized controlled study. Int J Obes (Lond). 2018;42(9):1680-1690.
Imaging of Childhood obstructive Sleep Apnea
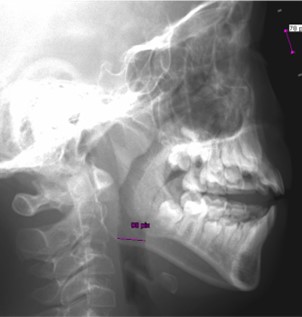
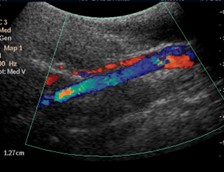
Craniofacial features obtained by radiography and ultrasound measurement of lateral parapharyngeal wall thickness is part of the comprehensive research program in studying childhood obstructive sleep apnea.
Representative publications:
- Yuen HM, Chan KC, Chu WCW, Chan JWY, Wing YK, Li AM, Au CT. Craniofacial phenotyping by photogrammetry in Chinese prepubertal children with obstructive sleep apnea. Sleep. 2023;46(3):zsac289.
- Yuen HM, Lai ACY, Liu EKH, Lee MC, Chu WCW, Chan JWY, Chan NY, Wing YK, Li AM, Chan KC, Au CT. Validation of the Sonographic Measurement of Lateral Parapharyngeal Wall Thickness in Childhood Obstructive Sleep Apnea. Nat Sci Sleep. 2022;14:2013-2021.
- Au CT, Chan KC, Zhang J, Liu KH, Chu WCW, Wing YK, Li AM. Intermediate phenotypes of childhood obstructive sleep apnea. J Sleep Res. 2021;30(3):e13191
Advanced Neuroimaging research in pediatrics patients
Our department has collaborated with Department of Linguistics and Department of Psychology in multiple competitive grants supported studies using neuroimaging to predict the language and cognitive outcomes in different groups of young patients. The titles of the funded projects are as follows:
- Neuroimaging, Cognitive and Life Functioning Outcomes in Patients with Haemophilia (GRF 2020/21)
- Using Neuroimaging to Predict Language Outcomes in Chinese-Learning Children with Cochlear Implants (GRF 2019/20)
- Using Advanced Neuroimaging to Predict Language and Cognitive Outcomes in Pre-Term Infants (CRF 2019/20)
Representative publication:
- Cheung YT, Ma CT, Lam HHW, Ling SC, Kwok K, Li CH, Ha CY, Yip SF, Wong RSM, Chu WCW, Li CK. Clinical, neuroimaging, and behavioural risk factors for neurocognitive impairment in Chinese patients with haemophilia: A multicentre study. Haemophilia. 2023;29(4):1074-1086.